Update: Formaldehyde denial vote set for next week

Since 2014, Salmonella cases in humans in the European Union have risen by 3%. In fact, according to the European Centre for Disease Prevention and Control (ECDC) and the European Food Safety Authority (EFSA), one type – S. Enteritidis – was the cause of 1 in 6 foodborne disease outbreaks in 2016.
At this point the ECDC and EFSA haven’t pinpointed the cause, but their report does note that S. Enteritidis, which accounts for 59% of all cases in 2016, is associated with the consumption of eggs, egg products and poultry meat. It also notes Salmonella in eggs caused the highest number of outbreak cases. Some experts believe the increase can be attributed to outbreaks in countries like Poland where withdrawal of the use of formaldehyde in feed has led to a Salmonella crisis. Following a nearly one-month consultation period, which was aimed at gathering comment on the proposed regulation to deny authorisation of formaldehyde as a feed additive, the European Commission has decided to proceed with a vote next week.
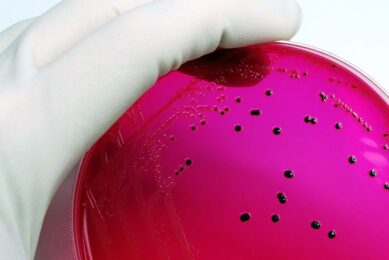
Salmonella: The facts
Salmonella cases in the EU are no longer in decline. In fact, cases in humans have increased by 3% since 2014. According to the ECDC and the EFSA, there were 94,530 human cases of salmonellosis reported in the EU in 2016 alone. Of those, 59% were attributed to S. Enteritidis, a type of Salmonella that is mostly associated with the consumption of eggs, egg products and poultry meat.
At this point, Marta Huga, EFSA Chief Scientist, can’t say what’s causing the rise. “Recent S. Enteritidis outbreaks contributed to a change in this trend in humans and poultry,” she said. “Further investigations by competent authorities in the field of public health and food safety will be crucial to understand the reasons behind this increase.”
However, further data shows that salmonella cases have increased by 73% (an increase from 0.7% to 1.21%) since 2014 where formaldehyde in animal feed for laying hens is no longer used.
Mike Catchpole, ECDC Chief Scientist, is concerned about the numbers. “The increase shown by our surveillance data is worrying and a reminder that we have to stay vigilant,” he said. “Even in a state of high awareness and with national control programmes for S. Enteritidis in place, there is a need for continuing risk management actions at the Member State and EU level.”
Formaldehyde denial vote set for next week
Following reclassification of formaldehyde from a biocide to a feed additive in 2013, the European Commission supported re-authorisation. However, since EU Member States were unable to come to an agreement on the re-authorisation, it expired in 2015. At that time the Commission proposed to deny re-authorisation. Concerns over the use of formaldehyde are not related to its use in feed in terms of animal and food safety, rather to occupational health risks. The Commission’s draft regulation to deny authorisation claims that the advantages gained by using formaldehyde as a feed additive are outweighed by the potential health risks for those who handle the substance.
Commissioner Thyssen, on behalf of the Commission, replied to Parliament questions on the subject, stating: “Formaldehyde is classified as a carcinogen” and “based on that classification, the substance falls within the scope of Directive 2004/37/EC on the protection of workers from the risks related to exposure to carcinogens or mutagens at work.”
“Consequently,” she went on the say, “employers are obliged to protect workers from exposure to this substance in accordance with the provisions laid down in that directive.”
A few months later, in another response, Ms Thyssen noted: “The planned amendment would not ban any use, including medical, of formaldehyde. In fact, the adoption of exposure limit values should be seen as providing a practical tool to assist employers to demonstrate that they comply with the general requirements of the directive which already apply in full to this carcinogenic substance.”
On 21 November, the European Commission opened up a consultation period to gather comments on its proposed regulation to deny authorisation of formaldehyde as a feed additive. The consultation period runs until 19 December 2017.
In the meantime, uncertainty over the outcome of the proposed regulation to deny authorisation has led several member states to stop using formaldehyde in animal feed. In Poland, where authorities withdrew support for authorisation early, the poultry sector has been facing a Salmonella crisis. Other countries, like Finland and the UK, temporarily re-authorised formaldehyde in animal feed pending a decision at the EU-level. So far, no substitute products for formaldehyde have been found.
The case of Poland
Amid the discussion, Poland has been facing what looks to be an intensifying Salmonella crisis. In fact, 2017 has been the worst year for outbreaks for the country in a decade. Thousands of cases have been reported, hundreds hospitalised, and the country has seen reduced exports on eggs and poultry products.
The crisis isn’t only limited to Poland, though. According to an epidemiological update ECDC issued in October, 7 member states reported 96 confirmed and 34 probable new cases associated with the multi-country outbreak of S. Enteritidis. Overall, the ECDC report shows that 797 cases were found to be associated with this outbreak. Of those, 376 were confirmed, and 291 were considered probable.
The investigation that followed the 2016 outbreak identified eggs originating from 3 Polish packing centres as the source of the outbreak. Following that and the subsequent implementation of control measures, the number of new cases fell sharply. However, since March 2017, the number of newly reported cases increased again, peaking at 38 in May. A second peak of 46 cases was reported in September. All outbreak-confirmed cases belong to 2 different WGS – whole genome sequencing – clusters: Cluster 175 and Cluster 360.
As of 5 October, according to the ECDC report, the bulk of the 200 cases – 155 confirmed and 45 probable – were reported by the United Kingdom (135 confirmed and three probable). The ECDC, however, does note that the UK is the only country that performs “routine and close to comprehensive WGS-based typing of Salmonella.” For this reason, they believe that the number of cases associated with the outbreak is most likely understated.
ECDC still investigating
In the assessment that followed the outbreaks, epidemiological, microbiological, environmental and tracing investigations identified eggs from Poland as the cause of the 2016 outbreaks. The ECDC is still investigating the cases from March 2017 on, but so far it doesn’t look good. According to a Rapid Alert System for Food and Feed (RASFF) report, the total number of RASFF notifications for salmonella in poultry meat products originating in Poland in 2017 is the same as the number of notifications originating in all of the 27 other EU countries combined.
Jim Bigmore believes the problem in Poland is multifactorial. Bigmore is CEO of Hysolv Ltd., a worldwide distributor for German biocide manufacturer Interhygiene. Bigmore also works part time for IDT Biologika as a salmonella vaccine specialist. The company is based in Germany. During his career, Bigmore has also been involved with the development and marketing of salmonella vaccines for Hoechst, and was responsible for global marketing at Elanco for their range of salmonella vaccines. He opened his own company in 2004.
In terms of what’s going on in Poland, Bigmore believes the underlying problem is more complex than just a withdrawal of the use of formaldehyde in feed. “Last year the price of eggs was extremely low, and this means that all egg farmers find ways of reducing costs,” he said. “One of the things they can do is they can hold onto their hens longer, so instead of the normal laying period, they will have an extended laying period.”
“This can extend an additional 10–20 weeks,” he continued. “This is a calculation you make as an egg producer. You get a drop in production, but this drop in income is offset by the fact that you don’t have to buy new birds.”
Bigmore pointed to last year’s egg prices, which were significantly lower than in previous years. “During 2016, the price for eggs was about 10-15% lower than in the preceding 3 years,” he said. “This was the time – May to October 2016 – that cases of phage type 8 were being reported.
Mr Bigmore believes that the outbreaks could also have something to do with vaccinations. “If you want to prevent Salmonella, there are really 3 legs to prevention,” he said. “There’s good management, there’s biosecurity, and there’s vaccination.”
He questions whether or not some producers chose to cut back on vaccines. When you use 3 doses, you’re more likely to get cross-phage protection, he explained.
“But if you use 2 doses, then what happens normally, is that the length of protection is less and you might not get this cross protection,” he said. “It doesn’t mean you won’t; it’s just not proven.”
“If you use 1 dose of the live vaccine, you’ll get even shorter protection,” he concluded.
Useful disinfectant
Formaldehyde, said Mr Bigmore, is an extremely useful disinfectant. In UK-based tests that compared different disinfectants used on-farm, He says formaldehyde performed well on dry surfaces in buildings. It’s also used in foot baths to help to further protect farms from pathogens.
“For use in buildings, formaldehyde has an absolutely crucial use,” said Mr Bigmore. “And this is that it’s a very cost effective, second disinfectant that is used on a farm.”
Typically, the first disinfectant is followed by an application of formaldehyde, applied as a fog using a low-pressure sprayer. “If you remove formaldehyde then really you’re forcing the farmer to either not have the second safeguard or you’re forcing them to use 2 disinfectants on one building,” he said.
“This, of course, will increase costs and the use of manpower.”
For now, formaldehyde registration as a veterinary hygiene product is ongoing, and the product can still be used, he said. Mr Bigmore could not provide comment on the use of formaldehyde in feed.
The Commission’s DG SANTE has scheduled a vote for the denial of authorisation at the next Standing Committee on Plants, Animals, Food and Feed (ScoPAFF) meeting, which is set for 19–20 December.
Join 31,000+ subscribers
Subscribe to our newsletter to stay updated about all the need-to-know content in the poultry sector, three times a week. Beheer
Beheer





 WP Admin
WP Admin  Bewerk bericht
Bewerk bericht